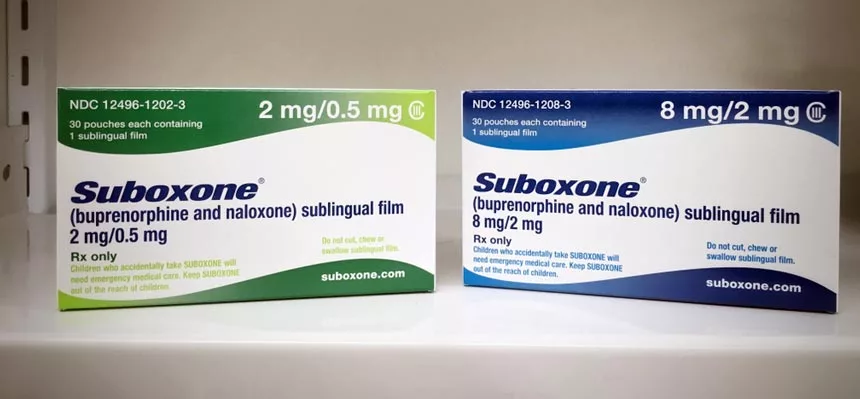
Finding Medication Assisted Treatment with Blue Cross Blue Shield
Table of Contents
- Finding Medication Assisted Treatment with Blue Cross Blue Shield
- Why is Suboxone Treatment the Gold Standard?
- Does Blue Cross Blue Shield Cover Suboxone Treatment?
- Suboxone Treatment: By Prescription Tier
- Payment Help for Suboxone Treatment
- Ask for the Generic Drug Version of Suboxone
- Will BCBS Insurance Always Cover Suboxone?
- Make Good Use of Your BCBS Deductible
- Does BCBS Pay for Private Treatment for Opioid Addiction?
- Get Your Addiction Under Control with Our Help
- FAQs About Suboxone Treatment with Blue Cross Blue Shield
- Medically Reviewed By
Maybe you have already tried everything in your power to kick your opioid addiction to the curb. If you find that you still are not making headway in your addiction treatment, it’s time to consider whether medication assisted treatment is right for you — namely, Suboxone. Now you need to know: does Blue Cross Blue Shield cover Suboxone treatment?
If your local drug and alcohol rehab offers this treatment, you need to know whether it will be covered by your health insurance. Here is the guide you need to navigate the healthcare system and figure out which treatments are covered for you!
Why is Suboxone Treatment the Gold Standard?
To many physicians and mental health providers, Suboxone treatment is the gold standard for opioid use disorder. According to Harvard Health Publishing, this medication can decrease the risk of fatal overdoses from opioids by as much as 50 percent. In addition, it is less likely that a person who is prescribed Suboxone will have a nonfatal overdose.
Most do not overdose on this type of prescription either.
Another important statistic to know is that treatment with buprenorphine (one of the generic components of Suboxone) reduced the risk of an opioid positive drug test by 14.2 percent. The same study showed that those on the medication were 1.82 times more likely to remain in treatment for their condition compared to those who received a placebo or no treatment.
Using Your Insurance Plan for MAT
Keep in mind that a general physician may have the ability to prescribe Suboxone treatment. However, they may also require you to put some effort into your recovery process. It may be a stipulation from your health insurance company or your doctor that you also engage in therapy. That could mean on an inpatient or outpatient basis.
This gives you the tools you need to face your substance use disorder and come out on the other side.
Whether you are looking for detox centers or a rehab facility, Find Addiction Rehabs can help. We specialize in helping you find a high-quality substance use treatment facility in your local area or wherever is best for you.
Does Blue Cross Blue Shield Cover Suboxone Treatment?
The good news is that many plans offered through Blue Cross will cover the cost of drug addiction treatment. However, the amount that will be covered depends on the specific provider you use, its location, and whether you decide to attend on an inpatient or outpatient basis.
The exact rules regarding Suboxone treatment depend on your state, but BCBS insurance has taken a big stand against opioid use disorder. We think you’ll find that they offer great insurance coverage for treating opioid addiction. Let’s take a closer look at what you can expect, state by state.
Anthem, Inc. and its Areas of Coverage
Anthem is a subsidiary of Blue Cross Blue Shield and it covers a wide range of states as an insurance provider, including:
- Colorado
- Connecticut
- Georgia
- Indiana
- Kentucky
- Maine
- Missouri
- New Hampshire
- Nevada
- Ohio
- Virginia
- Wisconsin
Anthem is taking the steps necessary to combat substance use disorder at the source. They require patients to use a single doctor and pharmacy, making it less likely that you will be able to play the system for access to more opioids. However, those already struggling with addiction can work with primary care providers to cover medication-assisted treatment.
This is particularly true for individuals seeking treatment in rural areas where an inpatient treatment facility may not be available.
If you do live in an area where minimal facilities are available, consider turning to us at Find Addiction Rehabs for help finding a facility that meets your needs in another area. We can help you find a program, whether that means you want an inpatient, outpatient, or detox center along with insurance verification.
Rhode Island and Elimination of Prior Authorization for MAT
One of the biggest hurdles for those already struggling to find quality substance abuse treatment is obtaining prior authorization before they can start the Suboxone or any other medication-assisted treatment. When already dealing with opioid withdrawal symptoms, it can feel impossible to navigate the healthcare system to obtain proper insurance coverage.
Blue Cross Blue Shield of Rhode Island recognizes the difficulty of obtaining treatment and aims to eliminate it at the source. There are no prior authorization requirements for the first ten days of your Suboxone treatment. This clears the barrier to entry that many people need so that they can put a stop to their opioid use disorder as soon as possible.
Other States Coverage Levels for Medications with BCBS
While these areas are the most forthcoming with their commitment to covering Suboxone on BCBS, they are not the only ones who offer it. Under the Affordable Care Act, Blue Cross Blue Shield must cover more behavioral health conditions. No longer are they allowed to deny individuals on the basis of substance abuse being a pre-existing condition.
This means that Blue Cross Blue Shield must cover at least some of your addiction treatment. Your premiums can be used to help cover mental health care, behavioral health, and substance abuse treatment.
Keep in mind that you may still have some out-of-pocket costs such as copayments, or you may have to pay your deductible before addiction treatment is covered. This is why many people wait until the end of the year to start treatment when their deductible is mostly paid for the year.
In-Network Providers for Blue Cross Blue Shield Insurance
The catch is that you must be using in-network providers that Blue Cross Blue Shield partners with in order for treatment to be covered. You can choose to see an outside provider, but you may have to cover the full cost of your treatment out of pocket.
Treatment facilities that are in the network have an agreed-upon service fee that minimizes the out-of-pocket cost for the insurance company. When you take advantage of services, they are not charged full price. An out-of-network provider may not have the same billing standards and could pass the full cost of treatment along to you.
If you are concerned about how you will find insurance coverage with Blue Cross Blue Shield, Find Addictions Rehab can help. We offer a section on our website to help you verify your insurance coverage. This allows you to figure out what type of treatment options will be covered by Blue Cross Blue Shield before you commit.
Suboxone Treatment: By Prescription Tier
While the other states are a bit less forthcoming about their initiatives to offer medication-assisted treatment, it’s good for your mental health to know what options are out there for you. Even without specific details on how Suboxone is offered in these other states, Blue Cross does recognize Suboxone treatment as a valid treatment for those in a drug and alcohol rehab or via their primary care doctor.
Suboxone is considered a tier 1 drug and a preferred medication. In most states, you are not required to have prior authorization for the initial dispensation of Suboxone. As long as you have already met your deductible or out-of-pocket maximum for the year, you should be able to receive medication-assisted treatment options.
This includes any doctor’s visits and lab work that must be done in order for you to continue receiving Suboxone, whether at a low dose or a higher one.
While the Affordable Care Act made some preventive medications available at no cost to Blue Cross Blue Shield customers, Suboxone does not fall into this category.
Payment Help for Suboxone Treatment
Even if you have excellent health insurance through Blue Cross Blue Shield, many people find that the treatment itself is cost-prohibitive. If trying to figure out how to pay for the gold standard treatment option is causing you stress and mental health concerns, there is good news.
There are prescription assistance programs that can cover part or all of the cost of your Suboxone if you qualify.
Suboxone has its own prescription payment program to help those who may not otherwise be able to afford this substance abuse treatment. Patients who do have insurance coverage are eligible to pay as little as $5 each month with two fills for new patients in the first month.
If you do not have insurance coverage and cannot afford treatment, you can save up to $170 on the monthly costs of the prescription.
These are great programs for those who may have let their Blue Cross Blue Shield coverage lapse or those who need some financial assistance to make taking Suboxone a reality for them. The benefit of the medication is worth the extra effort that it may take to figure out how to get the cost covered.
Ask for the Generic Drug Version of Suboxone
In states where insurance coverage may not allow you to take Suboxone, consider searching for a generic form. While this is the gold standard for addiction treatment of opioids, the generic often works just as well. It comes in the same sublingual film and contains two medications: buprenorphine and naloxone. Be sure to consult with your health insurance carrier to see if they will cover the generic version of Suboxone.
Oftentimes, the generic is a provider’s first choice as the cost is typically lower than the name brand. Unless your medical provider has a specific reason for prescribing the name brand, you may want to go ahead and ask for it to be filled as a generic which will be in a lower tier.
When might you need to consider the name brand over the generic? Brand name Suboxone is typically associated with a higher level of severe addiction, according to one research study. If your provider recommends Suboxone specifically, it may be because you were:
- Taking higher doses of opioids
- Consuming more alcohol in addition to drug use
- Taking in psychotropic substances daily
Will BCBS Insurance Always Cover Suboxone?
Many people worry that they will need to take on this prescription for the rest of their lives to keep substance abuse under control. The question is: will Blue Cross Blue Shield always cover the cost of your prescription? The answer depends on many factors, including how well you participate in your treatment plan.
Some people are able to eventually taper off their Suboxone treatment over time. If you are adjusting well to living with a substance use disorder, have good coping skills, and are ready to try to brave life without medication, this is great news! However, some people find that they like the accountability of Suboxone to deter them from taking more opioids when stress occurs or their mental health declines.
The important thing to note here is that you want to take the minimum effective dose. This means that you take only what you need. As you start to get your substance abuse under control, there’s a good likelihood that you can reduce the dose. Simultaneously, this may improve the financial burden of paying for your prescription.
Make Good Use of Your BCBS Deductible
If you want to try out Suboxone treatment to see if it helps you with your substance abuse, it can be a good idea to try it at the end of the year. Not only is this time fraught with stress from the holidays, but most people have already met their deductible or are close to meeting their deductible. Make good use of your health insurance coverage by trying this prescription once you have hit these payment thresholds.
Depending on your plan, you might find that more of your addiction treatment is covered, including stays in an inpatient rehab facility that makes use of medication-assisted treatment. You will get more intensive care, access around-the-clock to providers who can assist you, and access to prescriptions like Suboxone. All the while, you will be monitored by professionals.
This can be a great way to kickstart your recovery before you segue into outpatient treatment and behavioral health counseling.
If you are not close to hitting your deductible, you may consider meeting with a primary care physician who can prescribe Suboxone treatment. Otherwise, you may be hit hard with some unexpected bills for inpatient treatment.
Does BCBS Pay for Private Treatment for Opioid Addiction?
If you are unsure whether your treatment will cover private treatment for your opioid addiction, it is important to check with your provider prior to signing up. Some policies may be more apt to cover this type of private inpatient treatment center while others may not cover the claim. During private inpatient treatment, you will likely receive more features and benefits, some of which may not be covered.
Even if you have Blue Cross Blue Shield, you may have some out-of-pocket costs for this type of treatment. This might mean heftier copays. Alternatively, you may need to hit your out-of-pocket maximum for the plan before treatment will be covered.
If you aren’t sure what will be covered by your Blue Cross Blue Shield insurance plan, you can verify your insurance coverage levels through Find Addiction Rehabs. This service allows you to determine what will be covered and have a good idea of what costs you may incur for a particular treatment.
Remember that Suboxone can also be prescribed by some primary care physicians on an outpatient basis. This could minimize your costs, making it more likely that BCBS insurance will cover the prescription. While this is still private treatment, it is less expensive than an inpatient center.
Get Your Addiction Under Control with Our Help
Are you ready to take the first steps toward getting your opioid use disorder under control? Suboxone treatment may be a great first step to eliminate the likelihood of a fatal or nonfatal overdose, and many accredited rehabs offer Suboxone as part of primary treatment as well as through aftercare planning.
Find Addiction Rehabs has an experienced team to help you find the right facility, whether you are looking for inpatient, detox, or outpatient treatment. We even help you verify your insurance coverage before you get too far in the process.
Reach out to us today to learn more about which rehab facilities might be the best fit for you!
FAQs About Suboxone Treatment with Blue Cross Blue Shield
Does Blue Cross Blue Shield consider addiction a pre-existing condition?
Under the Affordable Care Act, insurance companies are no longer allowed to restrict coverage for mental health, behavioral health, or addiction treatment. It cannot be considered a pre-existing condition that limits your healthcare coverage. They must provide some assistance to help their members be the very best version of themselves without drug abuse.
What does Suboxone treat?
Suboxone treatment is used to help with the withdrawal symptoms that can accompany kicking your opioid addiction to the curb. It does not provide any type of high, so it is safe for anyone who is struggling with opioid abuse to take.
Is Suboxone different from methadone treatment?
There are many overlaps between methadone treatment and Suboxone treatment. First, both are used to treat opioid addiction and impact the same parts of the brain. Methadone is usually administered in a clinical setting whereas Suboxone is a prescription that you can take from the comfort of your own home. Many people prefer Suboxone because it does not require them to take more time off work to deal with their opioid addiction.
Deborah Tayloe is a freelance writer specializing in health and sciences. Deborah earned a B.S.Ed. in Secondary Education/English, accompanied by a Spanish minor. Her writing expertise allows her to craft engaging, impactful articles to help people be well.
In addition, she holds a fully accredited Certificate of Natural Medicine and is a certified Herbalist. Through her understanding of complementary medicine, Deborah helps medical professionals give people the information they need to embrace natural approaches to wellness.
When she’s not working, Deborah trains for 5K races and advocates for animal rights.